While the vast majority of pregnancies end in a normal birth, things do not always go to plan. You may be faced with anything from a premature birth to a Caesarean section. Dad Info gives you the facts on what can happen in the delivery suite
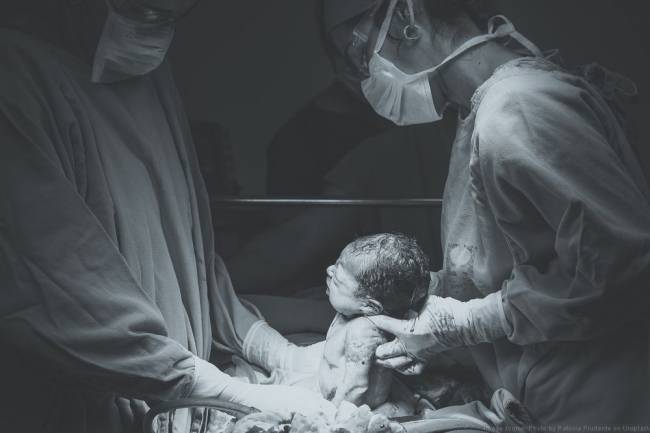
Advances in medical knowledge, diet and hygiene mean that your baby is highly likely to be born alive, 99.45 per cent in the UK. It is even more likely that your partner will survive, around 99.9 per cent. But there are other potential complications and sometimes, even after all the best preparation, medical intervention is needed to deliver your baby safely.
Helping at the birth: what can you do?
Premature birth
Premature birth is a term applied to a baby born any time before 37 weeks of pregnancy. Most pregnancies last around 40 weeks and the shorter the pregnancy the greater the risk that the baby will encounter problems.
There are many factors that can influence premature birth and currently around eight per cent of babies born in the UK are premature or underweight.
Babies born after 24 weeks may survive but will be kept in intensive care for a while. Two-thirds of those who survive grow up to be normal or have only mild to moderate problems.
Breech birth
A breech birth is where the baby has turned around so that her head is under your partner’s ribcage and her lower abdomen is closest to the cervix. If she moves into the breech position, she will be born legs or bum first instead of the normal head first position.
There are some methods used during the pregnancy to encourage the baby to turn but if they don’t work then your partner may be offered a Caesarean.
The baby can be delivered by a midwife or skilled obstetrician – a surgeon who specializes in pregnancy and birth – who can conduct a vaginal breech birth confidently, but you will need to check with your local hospital for details.
Induced labour
The midwife might suggest an induced labour:
- If your partner is more than 10 days past your due date.
- If your partner has pre-eclampsia or diabetes or certain other conditions.
- If the baby seems to be in distress.
- If your partner’s waters break but she does not have any contractions with the next 24 hours.
- If there is damage to the placenta.
Induction means using drugs or medical procedures to start the birth process. The main methods are:
- Membrane sweep – the midwife stimulates and/or separate the membranes around the baby from the cervix by moving her finger around the cervix. This causes a release of hormones which can kick-start labour.
- Artificial rupture of membranes – the midwife will break the waters to bring on labour
- Prostaglandin pessaries – this is a hormone-gel which is inserted into the women’s cervix. It will only work on around half of the women it is given to. Tablets can be used.
- Syntocinon drip – a drip that contains a hormone. which forces your partner’s womb to contract, beginning the movements of labour. The dose is started off gradually and built up to imitate how your partner’s body would naturally act.
Bear in mind that induction does not always work and, if it does, your partner may still experience a long labour.
Induced labours can also cause your baby stress, meaning that other interventions such as a ventouse, forceps or Caesarean delivery are more likely.
Tears
That’s tears as in rips, not tears as in crying.
Around one in three women experience a tear in the perineum (between the vagina and anus) when giving birth for the first time, and one in ten tear during subsequent births.
Although it sounds painful, most women experience nothing more than a slight burning sensation – although your partner may feel some discomfort for a few weeks after the birth.
There are several reasons why your partner might tear:
- If you’re having a big baby.
- If the baby needs to be delivered by ventouse or forceps.
- If the delivery is quick.
- If your baby is in an awkward position.
Whether or not the tear is stitched depends on how severe it is. Small tears are often not sutured as they heal quickly on their own. Larger tears might require a few stitches, which will be put in under local anaesthetic. The stitches will dissolve after a couple of weeks.
Serious tears, for instance might require surgery.
Your partner will be given painkillers to ease the discomfort.
Episiotomy
An episiotomy is a small cut of about two to three cm made between the vagina and anus to enlarge the vaginal opening. The procedure is conducted by a midwife or obstetrician to allow more room for the baby’s head to pass through. It may be necessary for a breech birth or if the baby’s head is too large.
- Episiotomies are normally carried out if it is necessary to speed up the delivery, for instance if the baby is in distress or if your partner is exhausted and can no longer push.
- Your partner will be cut under local anaesthetic when the head is crowning, and the cut will be stitched afterwards.
- The stitches will also be put in under anaesthetic, and dissolve after a couple of weeks. Your partner will be given painkillers to ease the discomfort.
It is entirely your partner’s choice as to whether she consents to undergoing an episiotomy and she should look into it well before the due date.
Forceps or ventouse (vacuum) extraction
If the labour is taking a long time and your partner is too exhausted or drugged to push, the midwife may suggest using a ventouse to help pull your baby out. This is a bathplug-shaped rubber cup that is attached to the baby’s head like a suction cup.
Although ventouse delivery can cause your baby to be delivered with a slightly stretched head, this only last for 24 hours and there should be no side-effects.
Forceps, instruments that look a little like salad tongs, can also be used to help pull the baby out. Again, they may cause your baby’s head to swell slightly for 24 hours.
Your partner may be given an episiotomy if either forceps of ventouse extraction is to be carried out.
Caesarean section
Around 20 per cent of British births are by Caesarean section.
They are given
- When the baby appears to be distressed and the midwife feels that the delivery needs to be speeded up.
- When the baby is in the breech position and cannot be delivered naturally.
- In emergencies, such as when the placenta becomes detached or your partner’s blood pressure is too high.
- An emergency caesarean may also be necessary if your baby is premature or when your partner or the baby is at risk of trauma.
How is a Caesarean performed?
During a normal Caesarean, (or C-section), your partner will be given an epidural (an injection into their spine) – she won’t be able to feel anything in the lower part of her body.
If it is necessary to deliver the baby in an emergency, there may not be time for an epidural and a general anaesthetic will be given.
- Most hospitals allow partners to be present during planned Caesareans but you may be asked to leave the room in the hustle and bustle of an emergency Caesarean.
- A screen is placed in front of your partner so that she (and you, if you don’t want to watch) can’t see what’s going on.
- Two cuts are made: one just above the pubic hairline and underneath that through the uterine wall. The baby is then lifted out through this incision.
- After the delivery, the incision will be stitched with dissolvable stitches and your partner will be given painkillers. The cut will take around six weeks to heal properly.
You should expect your partner to be kept in hospital for about three or four days, although some units are sending women home after 48 hours. Once you get your family home, make sure that your partner doesn’t lift anything and that she gets plenty of rest.
Post-natal infection
There is always a risk of infection, especially if your partner has had a Caesarean, a particularly long labour, or lots of examinations.
The most common is endometritis, an infection of the lining of the womb. It is easily treated with antibiotics but can cause pain and fever so you might need to take care of her and the baby while she recovers.
Post-natal haemorrhage
Some women have excessive bleeding after delivery when the womb doesn’t contract fully or bits of placenta haven’t been expelled. Sometimes a minor operation is necessary.